Loading content
24x7 Emergency & Critical Care
Loading content
REVIVE. RESTORE. REACH. - Rayalaseema's most advanced physiotherapy centre
Neuro, spine, and orthopaedic rehabilitation in Kurnool. We use robotic gait training and structured recovery plans to restore mobility and independence.

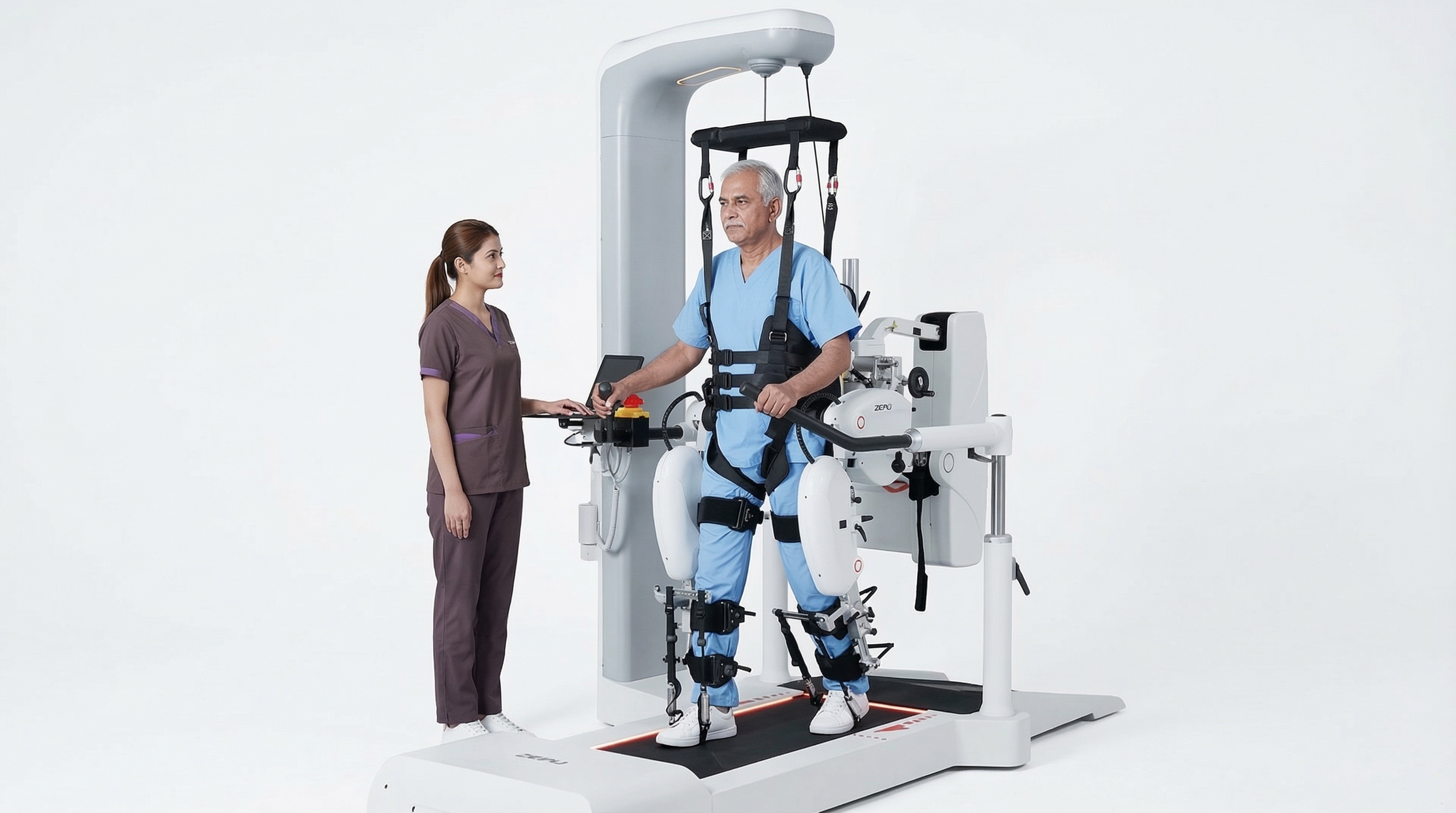
A body-weight-supported treadmill training system with robotic leg exoskeletons that guide and assist walking movement. Patients wear a harness and the robotic legs simulate normal gait patterns even before they can walk independently.
Who needs it
Stroke survivors with leg weakness, spinal cord injury patients, those with neurological conditions affecting gait (MS, Parkinson's), and post-surgical patients relearning to walk.
When
As soon as the patient is medically stable, even when unable to bear full body weight.
Why it matters
Provides up to 1000 repetitions per session of normal walking patterns, stimulating neural pathways far more effectively than manual-assisted therapy alone.
Key Benefits

Water-based rehabilitation performed in our purpose-built therapeutic pool. The buoyancy of water reduces body weight by up to 90%, allowing exercises that would be impossible or too painful on land.
Who needs it
Patients with arthritis, post-joint replacement, neurological conditions, obesity-related musculoskeletal issues, and those who are too weak or painful for land-based exercise.
When
After surgical wounds are healed, or for those who cannot tolerate land-based physiotherapy due to pain or weight-bearing limitations.
Why it matters
Water provides unique therapeutic properties: buoyancy reduces joint load, hydrostatic pressure reduces swelling, and the resistance of water provides strengthening without equipment.
Key Benefits

Upper limb robotic therapy system that detects attempted arm or hand movements and assists their completion. Patients perform interactive virtual tasks while the robot provides exactly the right amount of assistance needed.
Who needs it
Stroke patients with arm and hand weakness, traumatic brain injury patients, and those with upper limb neurological dysfunction.
When
Early in rehabilitation — can begin even when voluntary movement is minimal.
Why it matters
Detects and amplifies weak neural signals, providing intensive repetitive practice that strengthens the brain-to-muscle communication pathway through neuroplasticity.
Key Benefits
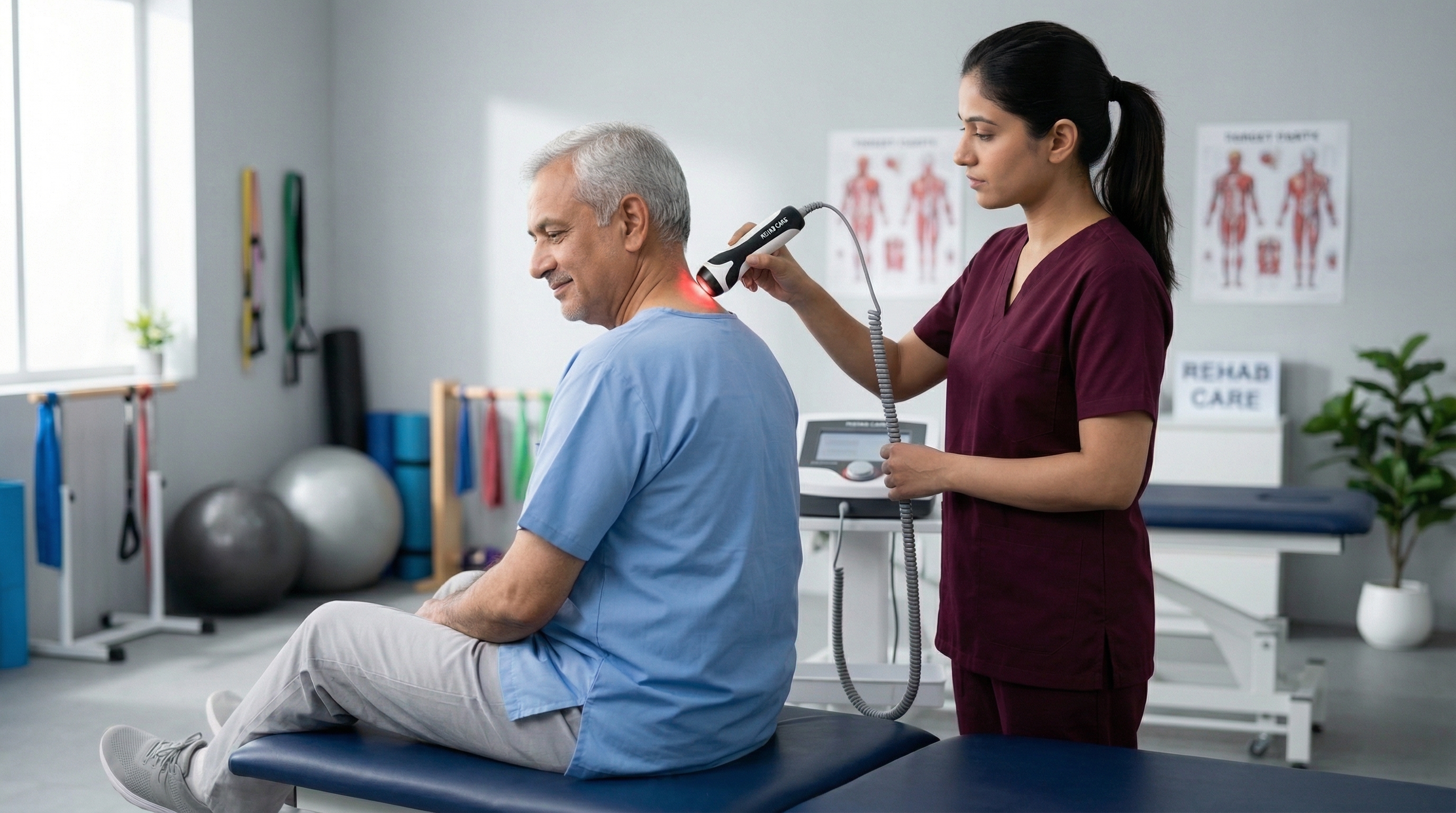
High-power Class IV therapeutic laser that penetrates deep into tissues, stimulating cellular repair, reducing inflammation, and relieving pain. Used for musculoskeletal conditions, neuropathic pain, and wound healing.
Who needs it
Patients with chronic back/neck pain, sports injuries, arthritic joints, neuropathic pain, tendinopathy, and slow-healing wounds.
When
As part of a comprehensive pain management program, often combined with physiotherapy and exercise.
Why it matters
Photobiomodulation (laser therapy mechanism) accelerates cellular repair at the mitochondrial level, increases local circulation, reduces inflammation, and provides analgesic effects — without medication.
Key Benefits
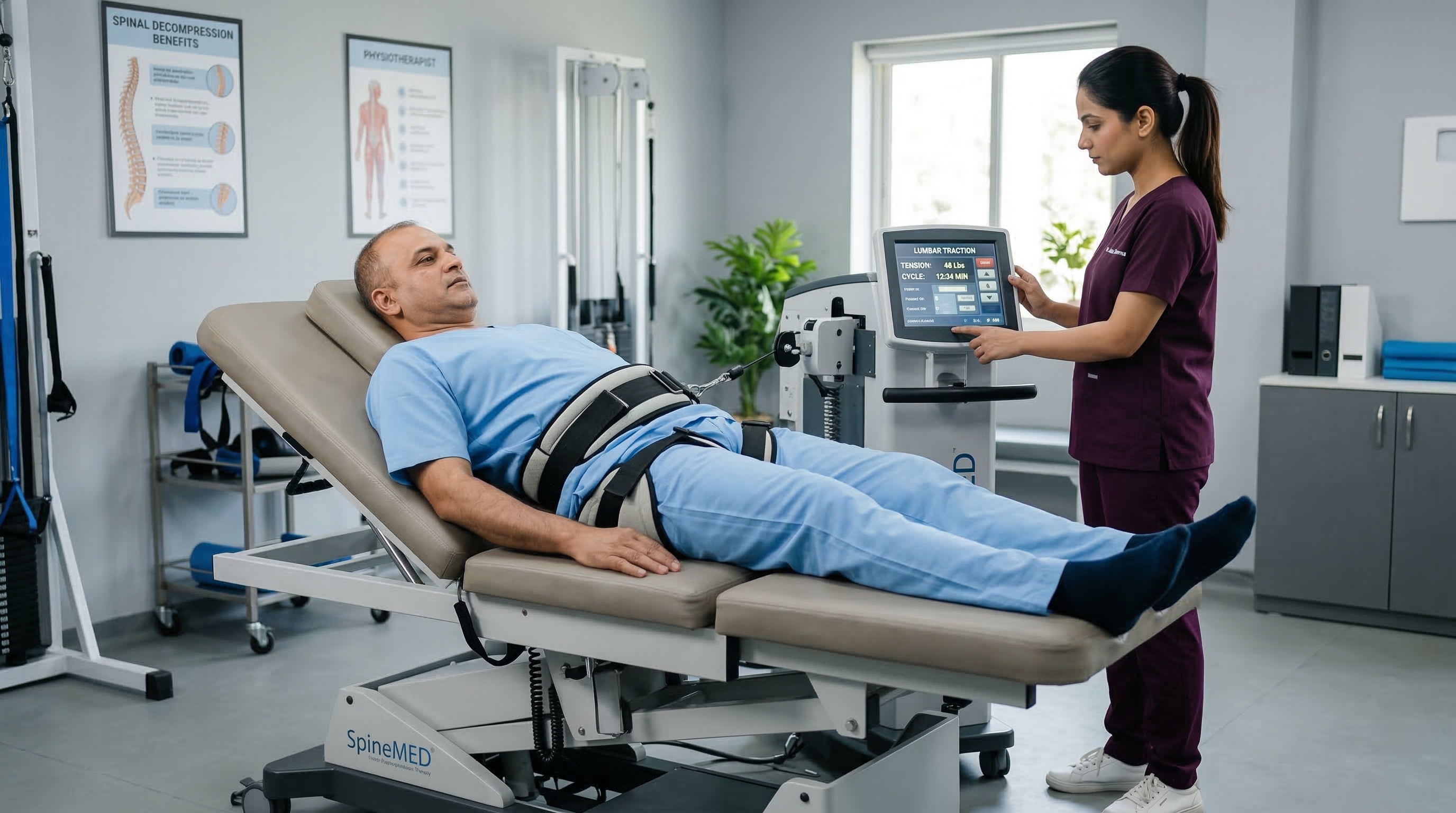
A comprehensive rehabilitation program for patients with complete or incomplete spinal cord injuries, combining functional electrical stimulation, robotic assistance, strengthening exercises, and daily living skills training.
Who needs it
Patients with cervical, thoracic, or lumbar spinal cord injuries from trauma, tumors, or spinal diseases.
When
After spinal stabilisation, typically within 1-2 weeks of injury for optimal neuroplasticity benefit.
Why it matters
Intensive early rehabilitation can convert incomplete to functional recovery in many SCI patients. Even in complete injuries, maximising independent function dramatically improves quality of life.
Key Benefits

An interactive virtual reality system that creates challenging balance and coordination tasks in a safe, controlled environment. Patients respond to virtual stimuli while standing on a balance platform, with therapists adjusting difficulty in real-time.
Who needs it
Stroke patients with balance deficits, elderly patients with fall risk, vestibular disorder patients, and those with cerebellar conditions.
When
After basic standing balance is established, as part of progressive rehabilitation.
Why it matters
Challenges the balance system in ways impossible with traditional therapy. Provides objective, measurable assessment of balance improvement and makes therapy more engaging.
Key Benefits
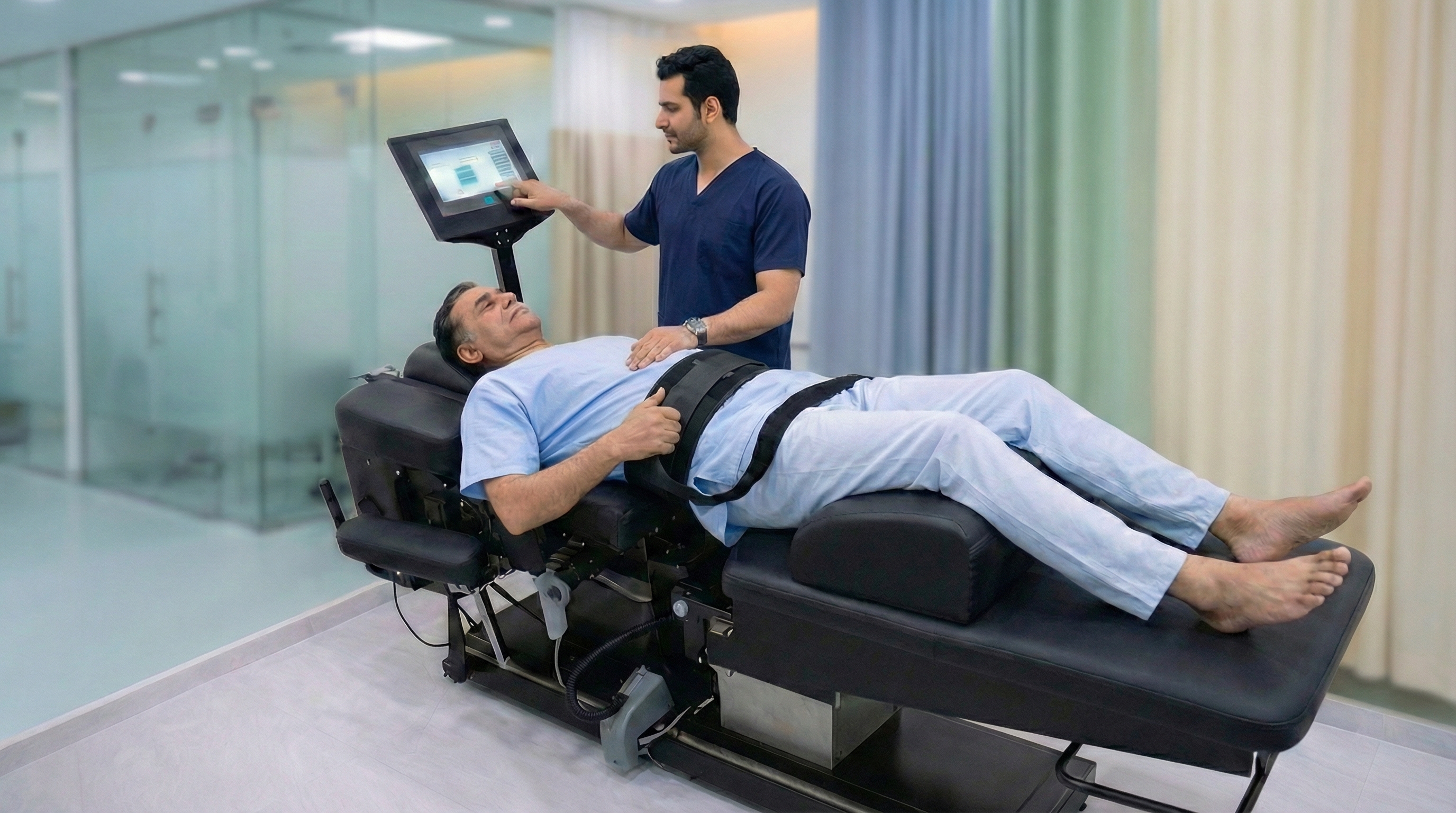
A computer-controlled traction therapy that gently stretches the spine to relieve disc pressure, reduce nerve compression, and promote disc healing — without surgery. The robotic system precisely controls angle, force, and duration for optimal results.
Who needs it
Patients with disc herniation, sciatica, chronic back or neck pain, and spinal stenosis who want to avoid or delay surgery.
When
After failure of conservative treatments (medications, standard physiotherapy) but before surgical consideration.
Why it matters
Creates negative intradiscal pressure, allowing bulging disc material to retract. Promotes nutrient and water reabsorption into dehydrated discs, facilitating natural healing.
Key Benefits

Prehabilitation (pre-surgery strengthening and optimisation) combined with post-surgical rehabilitation to maximise surgical outcomes and speed recovery.
Who needs it
Patients scheduled for elective spine surgery, joint replacement, or major orthopaedic procedures, and those in recovery from such surgeries.
When
Prehabilitation begins 4-8 weeks before surgery; post-surgical rehabilitation begins as early as day 1 after the procedure.
Why it matters
Patients who are stronger and more flexible before surgery recover faster, have fewer complications, and achieve better final outcomes. Post-surgical rehab converts a technical surgical success into a functional one.
Key Benefits

Structured rehabilitation programs for patients recovering from fractures, joint replacements, ligament injuries, and orthopaedic surgeries. Focuses on restoring strength, flexibility, and functional mobility.
Who needs it
Post-knee or hip replacement patients, fracture patients after cast removal, ligament reconstruction patients (ACL, rotator cuff), and those with chronic orthopaedic conditions.
When
Immediately post-operative for joint replacements; after fracture healing for other conditions.
Why it matters
Rehabilitation determines the final functional outcome after orthopaedic surgery. Even the best surgical result can be limited by inadequate post-operative rehabilitation.
Key Benefits

Specialised rehabilitation for sports and exercise-related injuries, combining injury-specific protocols with performance enhancement to return athletes to their sport safely and at peak performance.
Who needs it
Amateur and professional athletes, fitness enthusiasts, and active individuals recovering from sports injuries.
When
After initial injury management (RICE protocol) and medical clearance for rehabilitation.
Why it matters
Sports rehabilitation differs from general rehab in its focus on sport-specific movement patterns, performance metrics, and psychological readiness for return to sport.
Key Benefits

Child-focused rehabilitation services for neurological and orthopaedic conditions in children, using age-appropriate, play-based therapy approaches to achieve developmental and functional goals.
Who needs it
Children with cerebral palsy, developmental delays, brain injuries, spinal conditions, and orthopaedic issues.
When
As early as possible — early intervention produces the best long-term outcomes in paediatric neurological conditions.
Why it matters
The developing brain has greater neuroplasticity than adults. Early, intensive rehabilitation during critical developmental windows maximises functional outcomes for children.
Key Benefits

Specialised rehabilitation for elderly patients, addressing the unique challenges of ageing including reduced reserve, multiple comorbidities, and functional decline — with a focus on independence and quality of life.
Who needs it
Elderly patients recovering from stroke, fractures, joint replacements, and those with progressive neurological conditions like Parkinson's disease or dementia.
When
After any hospitalisation for acute illness or injury in patients over 65.
Why it matters
Older patients are at high risk of permanent functional decline after acute illness. Specialised geriatric rehabilitation addresses physical, cognitive, and social factors to maximise recovery.
Key Benefits

A multidisciplinary pain management programme combining interventional procedures, physical therapies, psychological support, and medication management for patients with chronic or complex pain conditions.
Who needs it
Patients with chronic back or neck pain, neuropathic pain, fibromyalgia, complex regional pain syndrome, and cancer-related pain.
When
When pain has persisted for more than 3 months despite conventional treatment, or when pain significantly impacts quality of life.
Why it matters
Chronic pain has biological, psychological, and social dimensions. A multidisciplinary approach addressing all dimensions achieves superior outcomes compared to single-modality treatment.
Key Benefits

