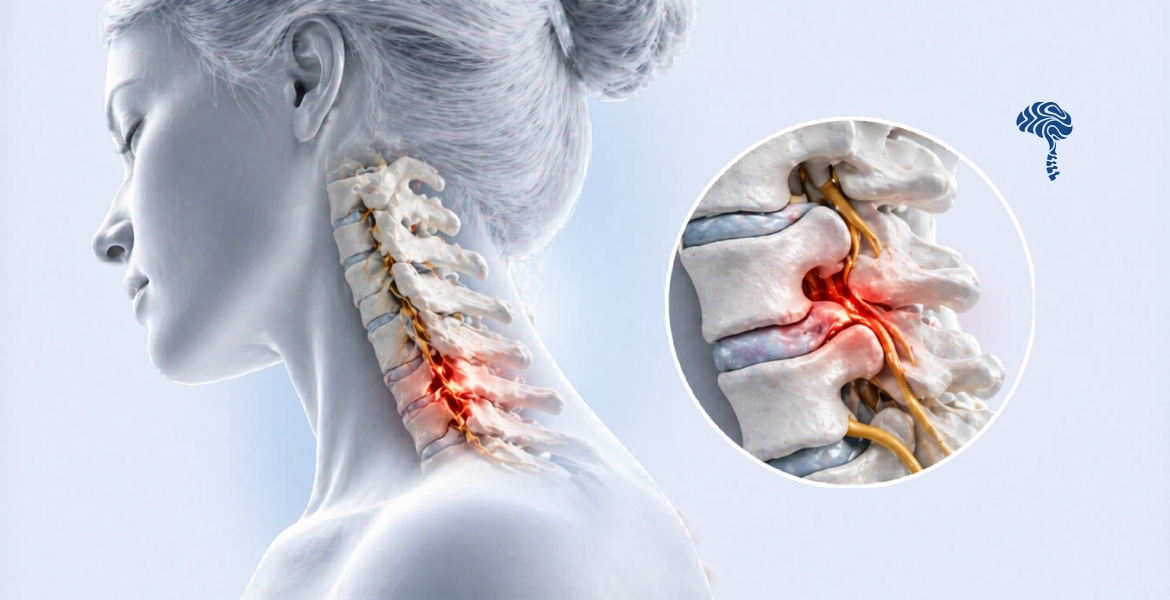
What Is Cervical Spondylosis?
Cervical spondylosis is a broad term for the age-related wear-and-tear changes affecting the discs, joints, and bones of the cervical spine (neck). It is virtually universal after age 60 on imaging — but many people remain asymptomatic. When structural changes compress neural elements, symptoms emerge.
The Spectrum of Disease
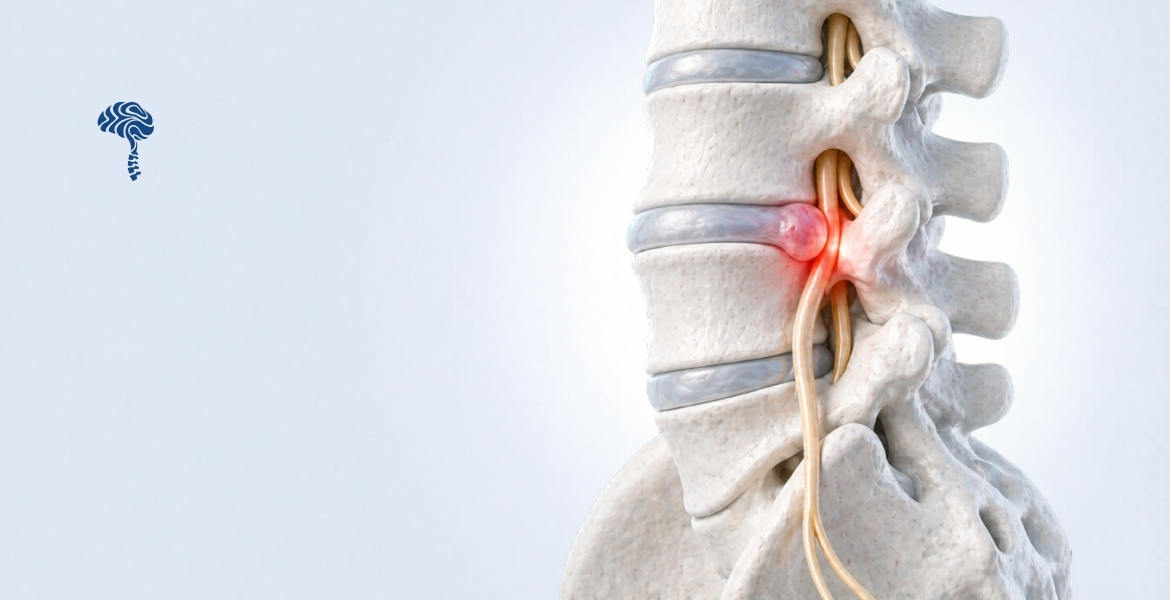
Cervical Radiculopathy
Compression of a nerve root causes pain, numbness, and weakness radiating into the shoulder, arm, or hand in a dermatomal pattern. C6 and C7 are most frequently affected.
Cervical Myelopathy
Compression of the spinal cord itself — the most serious manifestation. Features include:
- Clumsy hands, difficulty with fine motor tasks (buttoning shirts, writing)
- Unsteady gait, feeling of walking on cotton wool
- Upper motor neuron signs: hyperreflexia, positive Hoffmann sign, clonus
- In advanced cases: bladder urgency or retention
Cervical myelopathy is often insidious. By the time patients present, significant cord compression may already exist. Early recognition is critical.
Investigations
MRI cervical spine is essential to assess cord signal change (T2 hyperintensity indicates intrinsic cord injury). CT myelogram delineates bony compression. EMG/NCS differentiates radiculopathy from peripheral neuropathy.
Management
For Radiculopathy (Mild–Moderate)
- Physiotherapy — cervical traction, strengthening exercises
- NSAIDs, neuropathic agents (gabapentin, pregabalin)
- Cervical epidural steroid injection
Surgery for Myelopathy
Progressive myelopathy is a surgical condition. Decompression prevents further deterioration — recovery of lost function is variable. Approaches include:
- ACDF (Anterior Cervical Discectomy and Fusion) — gold standard for 1–2 level disease
- Cervical disc arthroplasty — motion-preserving alternative to ACDF
- Laminoplasty / Laminectomy — posterior approach for multilevel disease